Coeliac disease occurs in people who become sensitive to a protein called gluten in their diet. Gluten is found in wheat and other cereals and is normally a nourishing and harmless part of the food we eat.
However, if you have coeliac disease, gluten causes damage to the lining of your small intestine. This can cause problems with the absorption of nutrients and vitamins that we have eaten in the diet. Coeliac disease can be diagnosed at any age; from infancy to old age, but it is most commonly seen in children and young adults. The treatment, which is usually very successful, is to remove all sources of gluten from the diet.
Why does coeliac disease happen?
Although there has been considerable progress in our understanding of why people develop coeliac disease, many uncertainties remain. Like many illnesses, coeliac disease can run in families and the specific genes are now being identified. Currently genetic testing cannot be used to make a diagnosis of coeliac disease or identify whether you or a relative will develop the condition in the future.
How does gluten damage my intestine?
If we were to look at normal small intestine under the microscope, you would see vast numbers of tiny finger like projections sticking up from the surface. These are called villi and their purpose is to increase absorption of nutrients. In coeliac disease, the finger like villi look shorter and stubbier. In more severe cases, they can barely be seen at all, so the lining of the intestine looks quite flat. Doctors call this villous atrophy. We will see later how recognising villous atrophy is the key to making the diagnosis of coeliac disease. If patients with coeliac disease stop eating gluten, the villi grow back again.

A. In a healthy person, nutrients get absorbed by villi in the small intestine and go into the bloodstream.

B. In a person with Coeliac Disease , the villi have been damaged by inflamation, so fewer nutrients pass into the boodstream.
How many people are affected?
Over the past few years, it has become clear that coeliac disease is much commoner than we used to think. Recent research has shown that approximately one in 100 people in the UK have this condition. It is known to occur more frequently in certain countries and the world’s highest incidence is in the west of Ireland. The incidence of coeliac disease in people with first-degree relatives (parent, child, sibling) who have coeliac disease is 1 in 22, and with a second degree relatives (aunt, uncle, cousin) who has coeliac it is 1 in 40.
Most people who have coeliac disease don’t actually know they have it, but may still have some mild symptoms. Due to this, only 1 in 800 people have been properly diagnosed with coeliac disease in the UK. The implications for health of those with undiagnosed coeliac disease are unknown.
What symptoms might I expect with coeliac disease?
Interestingly there is a wide variation in the symptoms that people experience. In children, there may be diarrhoea, vomiting or a failure to gain weight. In adults, the disease comes to medical attention in a wide variety of ways. A common symptom is diarrhoea with bloating, or discomfort in the abdomen. Quite often, patients don’t have any symptoms that might relate to their guts but coeliac disease is suspected if tests show anaemia, or they are found to have thin bones (osteoporosis). Such diseases of the blood and bones may occur because patients cannot absorb iron, calcium and vitamins from their diet due to the damaged villi. In other cases, people lose weight for no obvious reason or just feel unwell in a rather vague way. Many patients have mild symptoms for months or years before seeing a doctor and only when they are correctly diagnosed and started on treatment do they realise how long they have been unwell.
How is coeliac disease diagnosed?
Having listened to your medical history and examined you, if the doctor suspects you may have coeliac disease, you will be asked to have some blood tests which will help to find out if you have the antibodies indicative of coeliac disease. These tests must be done while you are still eating gluten-containing foods. As we have seen, a doctor might consider a diagnosis of coeliac disease in many situations.
Fortunately, there is a simple test to look for antibodies in a sample of your blood that can reliably show whether you are likely to have coeliac disease. If the test is negative, it makes it very unlikely that you have coeliac disease. However, a positive blood test does not confirm the diagnosis beyond doubt. So if the result is positive, or in situations where there is still a possibility that you might have coeliac disease, your doctor will advise you to have a further test, to aid diagnosis, called an endoscopy.
What does endoscopy involve?
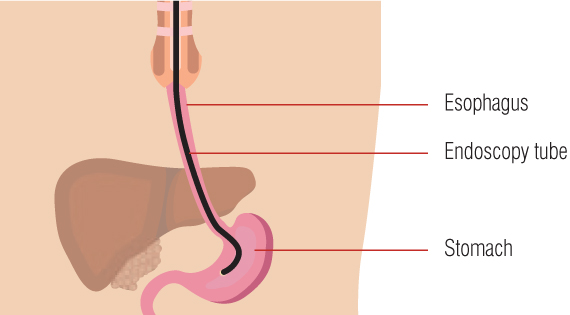
An appointment for endoscopy will be made either by your GP or your specialist and you will be given information about how to prepare for the test. On the day, a doctor or nurse will explain exactly what is involved.
Endoscopy involves passing a thin, flexible tube through the mouth and down to the small intestine where biopsies are taken. Neither passing the tube, nor taking biopsies, are painful although the procedure is not particularly comfortable. Your doctor will discuss with you the various ways in which the discomfort can be reduced and you will be able to choose the method that suits you best. Once obtained, the biopsy samples are sent to the laboratory to be examined under a microscope, which can show whether or not the villi are abnormal.
And if I do not fancy having endoscopy?
It is not compulsory to undergo any test or investigation, but it is important to appreciate that the only way to be absolutely certain of the diagnosis is by taking a biopsy from the small intestine by endoscopy. The treatment of coeliac disease requires a special diet for life and it’s absolutely crucial to be certain about the diagnosis.
How is coeliac disease treated?
As eating gluten causes the disease, the treatment is to avoid eating any food, which contains it. This means following a gluten-free diet for the rest of your life. If you are diagnosed with coeliac disease, the doctor will suggest you consult a dietician as sticking to a gluten-free diet requires knowledge about which foods contain gluten and how to maintain a balanced diet without wheat and the other cereals you must avoid. The dietician will provide written information to help you remember.
What exactly is gluten?
Gluten is a protein found in wheat, rye and barley. Gluten in flour is milled from these grains and found in many foods, especially bread, cereal and pastry.
What foods contain gluten?
Gluten is present in any foods that are made using wheat, rye or barley. Bread, pastry and cakes are all made with flour and contain large amounts of gluten. Breakfast cereals are often made from wheat, rye and barley with lots of other foods unexpectedly turning out to contain gluten. For example, flour is used as a thickener in many cooking sauces and barley is used in making all beers and lagers. Some foods occasionally get contaminated with small amounts of gluten during production or processing. Oats are not believed to be harmful to people with coeliac disease, but some products made from oats may contain traces of gluten, which make them unsafe to eat. It is worth learning to check the labels on such products to see if they are gluten-free.
Where can I find out more about what i can eat safely?
Coeliac UK (formerly the Coeliac Society) provides a large amount of information for people with coeliac disease. Your doctor will encourage you to become a member if you are diagnosed with coeliac disease. Coeliac UK publishes a list of gluten- free products in a handbook, which is updated every year. The list is also available to members on their website which also has links to other sources of information. They also publish a magazine that provides information about new products, recipes, social and educational events and research developments. You can contact Coeliac UK on 01494 437278 or the helpline on 0845 305 2060. Website: www.coeliac.co.uk
What can I eat instead?
There are a wide variety of alternative gluten-free products available for people with coeliac disease. A range of specialist substitute staple gluten-free foods is available on prescription from the doctor to help people with diagnosed coeliac disease adhere to a life-long strict gluten-free diet. The Advisory Committee on Borderline Substances (ACBS), an independent body advising the Department of Health, has approved a list of staple foods that form the basis of a nutritionally balanced diet. These foods include bread, flour replacement mixes, plain breakfast cereals containing no added sugar, pasta and crackers. Some of these foods are fortified with key nutrients such as calcium and fibre, which can be lacking in gluten-free diets. Mainstream manufacturers now make gluten-free foods and many of these, including luxury items, are available from supermarkets and health food shops. You should learn to check all foods and be aware of gluten-free sections of the supermarkets.

Can I rely on food labelling?
Current legislation requires food manufacturers to label foods so that all individual ingredients must be clearly stated. Most manufacturers label their products as gluten-free, but generally gluten should be listed as an ingredient where present. Restaurants are increasingly trying to help by indicating the use of gluten in dishes. However many restaurants currently do not label their meals and you may have to ask.
What happens if I eat gluten by accident?
This depends on how sensitive you are to gluten. If you only had mild symptoms originally then you will probably not feel ill if you consume some gluten by accident. This does not mean that you should not try to stick to your gluten-free diet as any amount of gluten can potentially cause inflammation in your intestine. Some patients are very sensitive to gluten and develop symptoms if they accidentally eat even very small amounts of gluten. For these people, it is even more important that they follow a strict gluten-free diet.
Why do I have to follow a gluten-free diet?
You are far less likely to have any symptoms if you follow a gluten-free diet. Most people who follow the diet say they feel healthier and more energetic. Following the diet will also reduce the risk of you developing future problems.
Will I need to stick to the gluten-free diet forever?
Yes. Coeliac disease does not go away although you will feel healthier if you are following the diet properly. You are far less likely to develop future problems if you stick to a gluten-free diet. Most people find it easier to follow the diet once they have got used to it.
What future problems might i have with coeliac disease?
Most people with coeliac disease stay healthy provided they follow a gluten free diet. There is a risk of developing problems such as a low iron count (anaemia) or thinning of the bones (osteoporosis) but these are far less likely if you eat the correct foods. If you do develop these problems, your doctor may put you on tablet supplements before starting the diet. Women with coeliac disease can have fertility problems but these usually resolve once the gluten-free diet has started.
Does coeliac disease increase your risk of cancer?
Having coeliac disease may increase your risk of having certain types of cancer. There is a rare form of tumour affecting the bowel, which does occur in a very small number of people with coeliac disease after many years, especially if they continue to eat gluten. If you have coeliac disease and adhere to the diet, you can expect the same life expectancy as anyone else.
Does my doctor need to check me regularly?
As you might develop problems in the future, it is worth keeping an eye on your health. It is recommended that you have a check-up once a year to ensure all is well. It is a good idea to have blood tests once a year to ensure you are not anaemic or have become short of vitamins and other nutrients. Your doctor may also arrange for you to have a simple scan of your bones from time to time to look for any sign that the bones have become thin so this can be treated early. People with coeliac disease are less able to produce antibodies to infections, so that vaccinations against pneumococal infections may be recommended.
Are any of my family likely to be affected?
Coeliac disease can run in families. As stated earlier, The incidence of coeliac disease in people with first-degree relatives (i.e. parent, child or sibling) who have coeliac disease is 1 in 22, and with a second degree relatives (aunt, uncle, cousin) who has coeliac it is 1 in 40. As the condition is easy to treat, there is no reason to worry about deciding to have children – unless you plan a very large family, as the chance is that your children will be unaffected. However, you may wish to let your siblings know that they may suffer from coeliac disease so they can have a check-up. Other more distant relatives, such as uncles, aunts and cousins are not more likely to be affected.
What research is needed?
 We need to know more about why people develop coeliac disease. This will involve more research on how the genes of people with coeliac disease differ from those who don’t have the condition. We also need to know more about how gluten causes damage to the intestine. Gluten-free products have become much better tasting in the last 5 years.
We need to know more about why people develop coeliac disease. This will involve more research on how the genes of people with coeliac disease differ from those who don’t have the condition. We also need to know more about how gluten causes damage to the intestine. Gluten-free products have become much better tasting in the last 5 years.
The information on this page about Coeliac Disease is based on the leaflet produced by CORE (a charity fighting gut and liver disease) who help fund research into gut and liver diseases..


